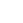
In-depth Analysis
Learning from COVID-19 experience
Enhancing service of LTCFs for the elderly
Since the Lunar New Year holidays this year, the fifth wave of COVID-19 outbreak has caused tens of thousands of infections. As of July 7, the total reported cases had reached 1.2 million and the death toll had risen to over 9000 in Hong Kong, with a death rate of 0.73%. More than 90% of the deceased were aged 65 or above. The long-term care facilities (LTCFs) for the elderly, also known as elderly homes, were in eye of the city’s deadly COVID storm as over 90% of them had an outbreak, a total of 30,000 elderly residents and over 8,000 staff members were infected. There have been vigorous discussions on the reasons behind the outbreaks of these LTCFs; some attributed the tragedy to the city’s anti-epidemic policy whereas some believed the lack of isolation facilities in these LTCFs should be held accountable for the outbreaks.
This article aims to analyse the conditions of LTCFs under COVID-19 with multiple perspectives including average living spaces in LTCFs, anti-pandemic supplies and facilities, nurse staffing ratio, staff-to-resident ratio, vaccination arrangement and the collaboration between LTCFs and the healthcare system. Learning from the policies and actions taken by the foreign countries in Europe and the US in administering outbreaks in the LTCFs, suggestions will be made to better prepare ourselves for possible crisis of the same kind in the future.
Stringent measures tapered impacts of the first four waves
Elderly residents in the LTCFs are usually with poor physical health and low mobility. Chronic illnesses and weakened immune system have caused them to be considered as high-risk groups for COVID-19. Together with the extreme high density of the LTCFs, there is a high chance of institutional outbreaks. Elderly also has high risk of several disease or even death from COVID-19.
The LTCFs in Hong Kong succeeded in avoiding casualties in the first two waves of pandemic. In July 2020, the outbreak of the third wave caused 136 reported cases and 30 deaths among the LTCFs, with a death rate of 22.1%. In October of the same year, the fourth wave induced 91 infections within the LTCFs and 11 elderly residents died with a death rate of 12.1%.
In the early stage of the pandemic, many LTCFs in Europe and the US encountered serious outbreaks, leading to a large number of infections and high death roll. Learning from their critical consequences and our fight against SARS in 2003, the government and the LTCFs have imposed strict anti-pandemic measures to protect elderly residents from contracting COVID-19. It was glad that the overall condition was under control in the first four waves despite several infection outbreaks observed in some of the LTCFs.
Anti-epidemic measures of LTCFs
Before the pandemic
- Requiring a nurse or a health worker to perform duties of an infection control officer, who oversees prevention and control of epidemic-prone diseases
- Providing Visiting Medical Practitioner Service to the residents of all private and self-financing LTCFs, as well as training on healthcare service and infection control to their staff
- Offering assistance to residents of subvented and private LTCFs by Community Geriatric Assessment Teams under Hospital Authority (HA)
- Specifying a list of infection control measures under the "Code of Practice For Residential Care Homes (Elderly Persons)" (The Code)
Human resources
- Starting from 2020, the Social Welfare Department (SWD) has provided special allowance for manpower support to compensate the extra expenses of the LTCFs in making necessary staff arrangement (including hiring of temporary staff/relief staff or internal deployment of staff to work overtime) under the special circumstances of COVID-19 outbreaks.
Anti-epidemic supplies and facilities
- The SWD has been distributing surgical masks to all staff of the LTCFs
- The SWD has been providing special allowance in purchasing personal protective equipment, sanitizers and disinfectants.
- In May 2020, the SWD launched the Anti-virus Coating Spray Subsidy to support the LTCFs to give their premises an anti-virus coating spray.
- In December 2020, the SWD launched the Time-limited Programme on Enhancing Infection Control and Ventilation of Residential Care Homes to enhance the infection control and improve their ventilation of the LTCFs of the territory.
- The Charities Trust of the Hong Kong Jockey Club distributed subsidies to the LTCFs to purchase equipment for improving ventilation.
- The Hong Kong PHAB Association Jockey Club PHAB Camp in Pok Fu Lam and Helping Hand Cheung Muk Tau Holiday Centre for the Elderly in Wu Kai Sha were reserved as isolation facilities for the close contacts of the elderly residents of the LTCFs to conduct quarantine.
Guidance to the LTCFs
- Reinforcing guidance to the LTCFs by the Centre for Health Protection and the SWD, including advice on enhancing infection control; improving personal and environmental hygiene; proper management on visiting arrangement, admittance of new residents or returning of recovered residents or staff from hospitals; handling suspected and confirmed cases and their close contacts; and enforcing the arrangement of on-site quarantine / isolation
- Suspending visiting arrangement to the LTCFs and limiting residents outing
Regular testing and vaccination requirement
- Starting from July 2020, all staff of the LTCFs has to conduct regular virus testing. The regular testing was changed to compulsory in November of the same year. A special allowance of HKD200 per month is distributed to the staff that receives compulsory testing.
- In early 2021, priority was given to the elderly for vaccination against COVID-19. Volunteering virus testing was also offered to residents of the LTCFs.
- Prioritized implementation of Vaccine Pass to the LTCFs requiring all staff to be vaccinated against COVID-19.
Insufficiency of the current protective measures under Omicron
Under the fifth wave of the pandemic, the number of infections and patients falling into critical conditions among LTCFs soared due to the high transmissibility of the Omicron variant. Local LTCFs were severely struck with the previous anti-epidemic measures. Such conditions further exposed some of the deep-rooted shortcomings of the elderly LTCFs policies, adding extra burden to the overloaded public healthcare system.
According to a research focusing on six European countries (Austria, Denmark, Germany, Ireland, Spain and Sweden), the infection rate of the entire population of a society is in proportion with the infection rate among elderly residents living in the LTCFs. In other words, the more infected cases in the community, there would be more infected elderly residents in the LTCFs. Since the first COIVD case in Hong Kong, the society had been maintained a low infection rate. However, most of the anti-epidemic measures only targeted at blocking virus spreading into the LTCFs. It is therefore expectable that the LTCFs would be severely hit and put under a difficult circumstance once the virus entered their gates.
Cramped living condition hinders Omicron prevention
A report from the Organization for Economic Cooperation and Development pinpointed that the population density of the LTCFs and the death rate of being infected by COVID-19 are highly correlated. In Hong Kong, the living conditions of the LTCFs for elderly have long been criticized. The minimum living space per resident as stated in law is only 6.5 square meters, which is around the area of half of the parking space for private cars. The living space per resident includes the elderly resident’s bed, personal storage cabinet, daily living space, public area, rehabilitative training space, corridor, washroom, kitchen and dining room. In addition to resident’s walking aids or wheelchair, it is conceivable how crowded and compact it is for elderly to move around and exercise inside the LTCFs.
Although the government has proposed amendments to bills to the Legislative Council this year to increase the minimum floor area per resident of care attention home and self-care hostel/aged home to 9.5 square meters and 8 square meters respectively, LTCFs in the city will reach the aforementioned standard no sooner than 2030 because of the 8-year transitional period. Whether 6.5 square meters or 9.5 square meters are both insufficient in terms of living space per resident in LTCFs even under normal circumstances. The densely packed environment of the LTCFs thereby provided an ideal condition for virus transmission when facing a highly contagious disease.
Another point that is worth our concern is the spatial configuration of the LTCFs: there are no individual rooms in most of the LTCFs. Instead, three or more residents share a room. For private LTCFs, open plan is widely adopted, and the beds are separated only with 1.2 meters tall partition boards. Social distancing measures to prevent droplet and bacterial transmissions are rare in both shared rooms and partitioned living space. While the government is calling for maintaining a social distance of 1.5 meters, frail residents in the LTCFs could not even stay 1 meter apart.
Shortages of protective equipment and manpower cause adversities
In the most difficult times of the pandemic, a number of LTCFs reported that they were in lack of medical supplies like protective clothing, face shields, rapid antigen test (RAT) kits and even oxygen supplies needed for first aid under emergency conditions. The shortages were most critical in the early stage of the pandemic as the SWD only provided financial subsidies to the LTCFs for purchasing medical supplies in the market themselves but not contacting wholesalers for bulk purchases and logistical arrangement when the whole city was in a situation of panic buying. The LTCFs had to arrange extra workforce for purchasing the supplies and thus dragging other services behind.
The medical equipment would not be useful without manpower from utilizing them. Review reports of the foreign countries recognized staff-to-resident ratio, especially the ratio of nurses to residents in elderly LTCFs, has a direct impact on the infection and death rates of the elderly residents. Research in the United States discovered that every 20 minutes increase in nurse staffing is associated with 22% fewer confirmed cases and 26% fewer COVID-19 death. Although LTCFs have to take care of frail elderly, there is no requirement under the current law stating the necessity of having a nurse station at the LTCFs. According to the Code, no enrolled or registered nurse is required if a health worker is on duty in a care and attention home or aged home. The Working Group on the Review of Ordinances and Codes of Practice for residential care homes of the SWD suggested raising the legal manpower requirement of the LTCFs, demanding at least one nurse to be on duty for 8 hours in the daytime every day in care and attention home. The proposal on bill amendment is anticipated to be put into effect within this year to take the first step of progress in enhancing the professionalism of the caretakers in the LTCFs.
Other than nurses, manpower of the LTCFs usually consists of care assistants, care workers, and health workers. Clerks, drivers, workers and chefs in the LTCFs are considered as care assistants. Under the law of Hong Kong, the manpower requirement varies in care and attention home and aged home according to different periods.
The residents for care and attention homes are elderly with poor health, declined physical capabilities, and those in need of assistance for activities in daily living. The Code stated that the minimum manpower requirement in the daytime shift of the care and attention home of the above example should have 3 staff looking after all frail elderly residents. They include elderly with low mobility and in need of using walking aids or wheelchairs, bedridden elderly in need of personalized care, elderly patients with dementia showing risks of wandering, elderly requiring assistance for activities in daily living such as eating, excretion, hygiene as well as elderly with nasogastric tube or urinary catheter. The overnight shift even only involves two staff taking care of all the elderly resident of the LTCFs. Having only 1 staff to take care of 20 elderly with low mobility is already an arduous task, not to mention the hardship of offering care service to frail elderly without self-care ability. From the above illustration, the staff-to-resident ratio of the LTCFs in Hong Kong is inadequate in providing quality care service to residents with personalized or special healthcare needs.
Apart from the problem of insufficient manpower as required in the Code, it is also challenging for LTCFs to recruit suitable personnel. Referring to the information from the Elderly Services Association of Hong Kong, the SWD and the Hong Kong Council of Social Service, labour shortages in subvented and private LTCFs in 2021 were 25% and 17.6% respectively. Currently, there are around 45,000 people working in LTCFs, with a manpower shortage of 20%, which means around 11,000 more workers are needed. To fulfill the legal manpower requirement and practical needs for operation, LTCFs would recruit part-time worker through job intermediary agencies. However, part-time workers are not a stable source of manpower as they flow between different LTCFs to work. These workers do not have enough understanding towards the working environment and the tempers or habits of the residents. This would inevitably affect the care service quality of the LTCFs and hinder their planning and training of manpower in the long run.
During the peak of the fifth wave of the pandemic, the problem of manpower shortage was further intensified as the staff members of the LTCFs would need to compel with the government regulations of quarantine, isolation, restriction-testing declaration or compulsory testing notice. Staff members would need to acquire a negative result in the polymerase chain reaction (PCR) test before returning to work in the LTCFs. As infection among elderly residents and staff continues, workers in the LTCFs are in the states of frustration and helplessness with low level of team cohesion. Despite that, the government has not classified COVID-19 as an occupational disease, leaving the need to address the mental health of the staff of the LTCFs.
Low vaccination rate and disconnection with the healthcare system
The difference in COVID-19 outbreaks between the LTCFs in Hong Kong and that in Europe or the US is the timing of launching the mass vaccination to the public. When COVID-19 was spreading rapidly among the LTCFs in Europe and the US in 2020, COVID-19 vaccines had not been successfully developed. This led to a huge number of patients in critical conditions or death cases from the LTCFs. On the contrary, Hong Kong had launched the vaccination programme in early 2021 and elderly were among the first to get the vaccine. Nevertheless, the vaccination rate among elderly was only 20% by the time of the fifth wave, resulting in high death toll among the elderly residents as they developed serious illness after being infected. There is no doubt that the society should respect the elderly’s own will in taking the vaccine or not, but the government should not solely accuse elderly’s personal choice as the reason leading to the low vaccination rate. Instead, the government should closely investigate and analyze the factors behind and then adopt a problem-oriented strategy, providing accurate and appropriate information for the elderly and their family members to make decision on vaccination.
Review reports from Europe and the US also pointed out that local government should develop and reinforce the partnership and cooperation between LTCFs and the healthcare system. Through establishing a set of guidance and a mechanism, together with the reinforcement in legislation, the public healthcare system can efficiently deploy manpower and resources to support the medical treatments needed for the elderly residents. In mid-February of this year, the HA reported that it was heavily burdened as LTCFs sent patients with mild symptoms to Accident and Emergency Department and rejected discharged elderly from returning to the LTCFs. The LTCFs sector responded and explained their dilemma as they could not spare extra manpower and protective equipment to look after discharged elderly who are still with abilities to transmit the virus to other residents. To prevent outbreak in the LTCFs, they had no choice but to refuse receiving discharged patients. The healthcare system and the LTCFs sectors held two very different standpoints in response to the crisis.
Since the SARS in 2003, the SWD required each elderly home to appoint one staff to be the infection control officer, in charging of infection control arrangements. However, there is not enough attention given on how to establish a mechanism to foster the communication and coordination between the LTCFs and the healthcare system in case of potential outbreak to provide appropriate medical care to the elderly patients while avoiding putting extra burden to the hospital system. In recent years, the society started to advocate a medical-social collaboration model, concentrating on development of primary care on a community level, for example, the District Health Centre Scheme, and the Dementia Community Support Scheme which provides support services to elderly persons with mild or moderate dementia. But such advocacy has not included the LTCFs sector. Visiting Medical Practitioner Service and the service from Community Geriatric Assessment Teams under the HA are the only backup supports for the LTCFs. During the most critical days of the pandemic, quite a number of elderly residents could neither be admitted to the hospital nor receiving medical treatment from the visiting medical practitioner but stuck at the LTCFs without any medical support.
While the hospitals could not handle an enormous number of infected patients, the infected elderly and their close contacts could only stay in the LTCFs for isolation and quarantine. However, given the conditions, facilities, and manpower of the elderly LTCFs, were they equipped with capabilities to become a suitable place for quarantine and isolation? Could they effectively separate infected patients and non-infected residents to prevent cross infection? The LTCFs sector reported that number of infections in LTCFs continued to rise despite their greatest effort to separate infected residents from the non-infected ones under limited resources and manpower.
Are setting up specialized coordinating units and LTCFs contact officers, case hotline, as well as establishing a platform for regular communication between organizations under each hospital cluster feasible and effective measures to coordinate for the treatment and isolation arrangements for the elderly residents? To achieve a seamless partnership between healthcare sector and social welfare sector for enhancing the medical care provided to the elderly residents, it is of paramount importance for the government to take the leading role, then coordinating between the SWD, the HA, and the LTCFs sector.
A Comprehensive review on the Residential Care Homes (Elderly Persons) Ordinance
In previous years, the government excused itself from reforming the Residential Care Homes (Elderly Persons) Ordinance that was established 20 years ago. It claimed that a reform would cease the private LTCFs from operation as their financial burden would then be greatly increased. The current situation of the LTCFs sector includes problems from different aspects: land, resources, regulatory complication, and the long-term planning of the sector. The fifth wave of the pandemic revealed the deep-rooted problems of the policies for regulating LTCFs. In face of the Silver Tsunami in Hong Kong, demand for care service in LTCFs will continue to spike. Now is the time for reformation before the current situation gets worsen.
Early this year in March, the Labour and Welfare Bureau set up an inter-departmental task force to review and strengthen the LTCFs’ capabilities in pandemic fight. It is hoped that the government could examine and reform LTCFs, investigating issues including land planning, manpower training and specialization, facilities and hardware requirement, staff-to-resident ratio, Pilot Scheme on Residential Care Service Voucher for the Elderly, affordability ratio between the government and the public, medical-social collaboration mode and all relevant aspects. A comprehensive enhancement in the care service enables frail elderly to live a more dignified and quality life in the LTCFs, and better prepares them to handle possible viral or contagious health crises in the future.
- Dykgraaf, S. H., Matenge, S., Desborough, J., Sturgiss, E., Dut, G., Roberts, L., McMillan, A., & Kidd, M. (2021). Protecting Nursing Homes and Long-Term Care Facilities From COVID-19: A Rapid Review of International Evidence, Journal of the American Medical Directors Association, 22(10), 1969-1988. https://doi.org/10.1016/j.jamda.2021.07.027.
- Frisina Doetter, L., Preuß, B., & Rothgang, H. (2021). Taking stock of COVID-19 policy measures to protect Europe’s elderly living in long-term care facilities. Global Social Policy, 21(3), 529–549. https://doi.org/10.1177/14680181211013717
- Grabowski, D.C. (2021). The future of long-term care requires investment in both facility- and home-based services, Nature Aging 1, 10–11. https://doi.org/10.1038/s43587-020-00018-y
- Li, Y., Temkin-Greener, H., Shan, G., & Cai, X. (2020). COVID-19 Infections and Deaths among Connecticut Nursing Home Residents: Facility Correlates. Journal of the American Geriatrics Society, 68(9), 1899–1906. https://doi.org/10.1111/jgs.16689
- Ochieng, N., Chidambaram, P., Garfield, R., & Neuman, T. (2021, Jan 14). Factors Associated With COVID-19 Cases and Deaths in Long-Term Care Facilities: Findings from a Literature Review. US: Kaiser Family Foundation. https://www.kff.org/coronavirus-covid-19/issue-brief/factors-associated-with-covid-19-cases-and-deaths-in-long-term-care-facilities-findings-from-a-literature-review/
- The Organisation for Economic Co-operation and Development. (2021). Rising from the COVID-19 crisis: Policy responses in the long-term care sector. https://www.oecd.org/coronavirus/policy-responses/rising-from-the-covid-19-crisis-policy-responses-in-the-long-term-care-sector-34d9e049/
- Thompson, D., Barbu, M., Beiu, C., Popa, L. G., Mihai, M. M., Berteanu, M., Popescu, M. N., The Impact of COVID-19 Pandemic on Long-Term Care Facilities Worldwide: An Overview on International Issues, BioMed Research International, 2020. https://doi.org/10.1155/2020/8870249
- Wong, K., Lum, T., & Wong, G. (2020, July 9). The COVID-19 Long-Term Care situation in Hong Kong: impact and measures. International Long-Term Care Policy Network. https://ltccovid.org/wp-content/uploads/2020/07/Hong-Kong-COVID-19-Long-term-Care-situation_updates-on-8-July.pdf
- 社會福利署(2020)。安老院實務守則。https://www.swd.gov.hk/storage/asset/section/2923/sc/cop_rche_chi_202101.pdf
- 立法會衞生事務委員會(2021年)。香港預防及控制2019 冠狀病毒病的措施(綜合檔案名稱:CB(4)600/20-21(04)),香港:立法會。
- 香港安老服務協會(2021年)。解決人力資源癥結 倡導行業專業化。安協薈刊,8-10月號。
- 立法會福利事務委員會(2022 年)。提升安老院及殘疾人士院舍質素的修例建議 (綜合檔案名稱:CB(2)77/2022(04)),香港:立法會。
- 立法會福利事務委員會(2022 年)。院舍抗疫工作(綜合檔案名稱:CB(2)177/2022(02)) ,香港:立法會。
- 勞工及福利局(2022年4月3日),局長網綕,院舍人手不足:不爭的事實。https://www.lwb.gov.hk/tc/blog/post_03042022.html